There are several types of glaucoma. Causes, symptoms, and people prone to it vary.
Angle-closure glaucoma
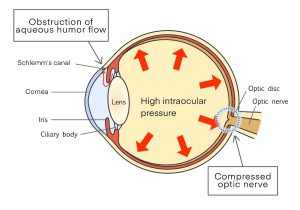
The outlet of the aqueous humor is called the angle. Angle-closure glaucoma is caused by an increase in intraocular pressure as a result of narrowing of the angle, which prevents the flow of aqueous humor.
- Acute type: Significant increase in intraocular pressure, accompanied by decreased visual acuity, eye pain, headache, and nausea
- Chronic type: may be accompanied by blurred vision especially at night or mild headaches
Women in their 40’s and older are 3-4 times more prone to the disease than men, especially those with farsightedness.
There are certain drugs that cannot be used for those diagnosed with angle closure glaucoma. Must check with your ophthalmologist regarding your glaucoma type and the drug’s should not be used or not.
Open-angle glaucoma
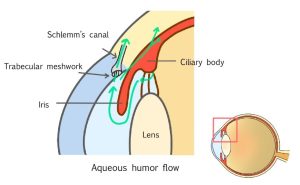
Even if the angle of the anterior chamber is wide enough, they may become clogged with trabecular meshwork. As a result, the increased intraocular pressure causes open-angle glaucoma.
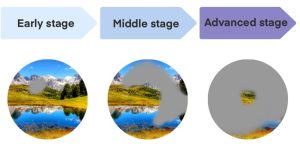
Intraocular pressure rises slowly, with almost no symptoms in the early stages. As the disease progresses, some areas of difficulty in seeing may appear and visual field defects may begin to occur.
Many diseases occur over the age of 40, and the rate increases with the age. It is said that it tends to be more common in people who are myopic originally. POAG occurs more frequently in eyes with myopia.
Normal tension glaucoma
In some cases, glaucoma develops even when the intraocular pressure is within the normal range of 10 to 21mmHg and is classified as part of open-angle glaucoma. It is caused by a weak structure of the optic nerve papilla, which cannot withstand even normal intraocular pressure and damages the optic nerve.
A previous study of several thousand people reported that glaucoma occurred in 5% of the population aged 40 years or older, and that more than 70% of them had normal tension glaucoma in Japan.
Secondary glaucoma
Secondary glaucoma is caused by the effects of another disease that was originally present. It may be caused by due to prolonged steroid medication eye drops, retinal diseases led by diabetes or etc.
Prolonged use of steroid application, oral medications, or eye drops can increase intraocular pressure, therefore requires an ophthalmologist’s visit.
Secondary glaucoma also includes increased intraocular pressure caused by trauma, corneal disease, or inflammation of the eye, which results in glaucoma.
Childhood (congenital glaucoma)
If the child is born with developmental abnormalities of angle, the intraocular pressure increases, and the optic nerve is damaged.
Occurs in about 1 in 30,000 people, the early-onset type occurs in approximately 80% of patients by the age of 1, while the late-onset type occurs in younger people in their teens to 20s, although the degree of the angle abnormality is less severe.